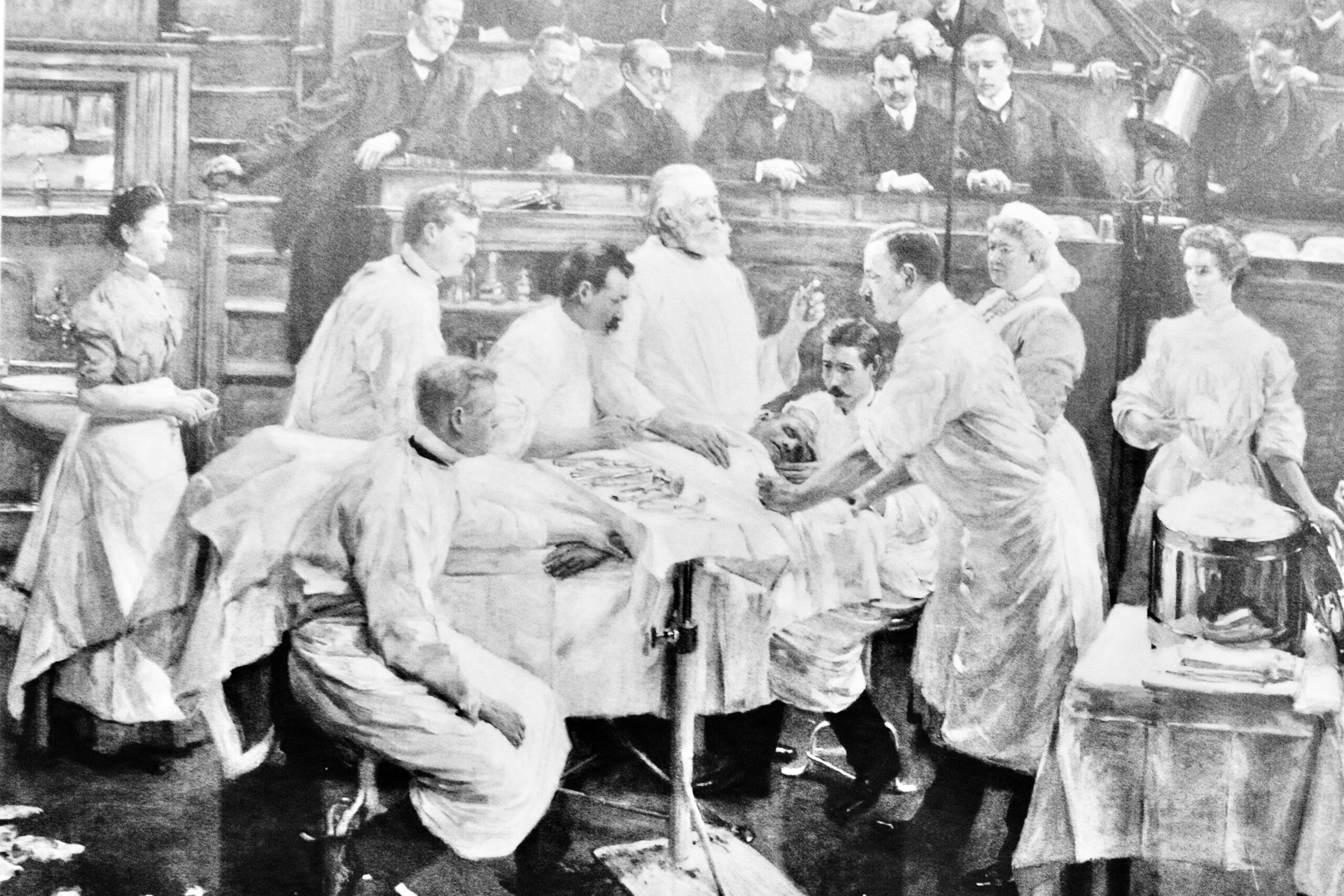
Saphenion®: The Endovenous „Saphena“ – views back into the Golden Twenties
Saphenion®: The Endovenous „Saphena“- We will try to give an overview of the historical development of the varicose vein treatment. You will agree after a short time with the words of Minkiewicz (1862): „Comparative studies of all surgical procedures recommended against varices“ (25) that „the quantity of some healing methods proposed in surgical and therapeutic practice against certain diseases either proves that the former has not yet been sufficiently researched or that the actual healing method is yet to be discovered. This applies to a large extent to varices and the usual „operation methods“ “ and we will try to describe the first therapeutical revolution from radical surgery to the endovenous therapy of varicose veins in the Twenties. We will show our ideas, mistakes, and experiences considering the historical development.
Our Keywords for this are:
History varicose veins therapy, endovenous/open surgery, sclerotherapy vs. Babcock – stripping, radical surgery vs. endoluminal ablation, beginning of endovenous therapy, last century discussion stripping / endovenous therapy.
Saphenion®: The Endovenous „Saphena“ – Introduction
Saphenion®: The Endovenous „Saphena“ – Almost 50 years ago, Dr. W. Lahl entered the Surgical Clinic as a training assistant. He was immediately entrusted with the care of varicose vein patients. Also, Dr. Ulf Zierau began his residency in 1988 at the Charitè with the radical therapy of varicose veins.
At that time, the patients were mainly treated as inpatients. The hospital stay was approximately 7 days.
The old-timers were glad that they no longer had to worry about the unspectacular clinical picture, the operations were without exception at the end of the surgery program. The boss appeared regularly in the room to ask what keeps me so long with the patient. He said: „It is a disease and not cosmetics“. He was most disturbed by small incisions. At this time, the saying still applied: „Major incisions, major surgeons – minor incisions, minor surgeons.
But what`s the reason – we had the Golden Twenties!
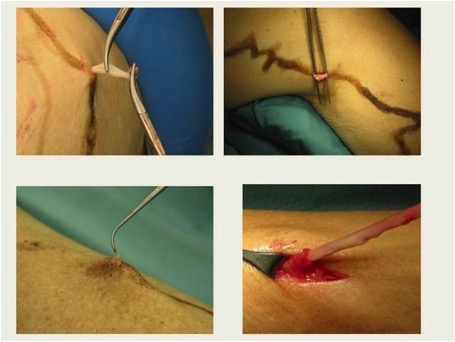
However, We have to add that the majority of patients were patients with pronounced chronic venous insufficiencies, often in combination with ulcer cruris. Cosmetic aspects were actually not in the foreground at that time. Even today, We remember the first operation reports, which were stereotypical: Skin incision hand wide below the groin, searching for the saphena and severing between ligatures…Then a button cannula was bound in and retrograde instillation of a calorose solution, a 60% invert sugar, took place. The patient lying under local anesthesia had to indicate as soon as he noticed a feeling of warmth in the ankle area. This completed the procedure and compression bandaging was performed. Ultimately, this procedure corresponded to the procedure proposed by Moszkovicz in 1927 – in the Golden Twenties (27).
Saphenion®: The Endovenous „Saphena“ – Were we already pioneers of endovenous therapy?
Looking back, We have to ask ourself whether we were among the pioneers of chemical endovenous therapy at the time, or whether the treatment was based on an antiquated procedure. Unfortunately, revascularization of the truncal veins and thrombosis due to the transfer of the high percentage solution into the deep vein system were possible complications. We therefore dedicated ourself to the stripping procedure after a short time. The existing, approx. 60 cm (23.6 inches) long original Babcock probes were, however, only conditionally suitable. They were too rigid as well as too short and the vein material often slipped over the probe olive. At that time, we were still far away from an invaginating or stage-appropriate stripping, the exhairese up to the malleolus was the rule. But – didn`t we know the old endovenous technique from the Twenties?
Saphenion®: The Endovenous „Saphena“ – Historical review
If you try to get an overview of the historical development of the varicose vein treatment, after a short time you agree with the 1862 of Minkiewicz „Comparative studies of all surgical procedures recommended against varices“ (25) that „the quantity of some healing methods proposed in surgical and therapeutic practice against certain diseases either proves that the former have not yet been sufficiently researched or that the actual healing method is yet to be discovered. This applies to a large extent to varices and the usual „operation methods“. In order to be able to appreciate the changes in dealing with the insufficient Saphena vein, which have taken place over the course of centuries, we have to take a look back into the more distant past.
Saphenion®: The Endovenous „Saphena“ – The last century
Descriptions and illustrations of varicose veins and their complications are already available from pre-Christian times as well as the following centuries. However, therapeutic measures consisted mostly only of relieving interferences with complications.
The basement of our knowledge of venous circulation was laid by Farbricius Aquapendente, who discovered the venous valves around 1584 and also pointed out the functional importance of these valves for venous circulation. His student William Harvey incorporated this early knowledge into his scientific concept of the entire bloodstream. Two centuries later, Tomasso Rima first described the role of Saphena magna (GSV) varicosis as a trigger of venous reflux and concluded logically that Saphena must be stopped at its junction. This demand for a radical OP was not enforceable in the 18th. century (2,3)
Saphenion®: The Endovenous „Saphena“ – Pro and contra saphenectomy
Only with the introduction of anaesthesia, anti- and asepsis in the middle of the 19th. century you come across an almost unmanageable number of different treatment proposals to eliminate the pathologically dilated saphenous septum and the varicose side branches. For a long time though, leading surgeons generally spoke out against surgical intervention.
Johann Friedrich Dieffenbach (4), who held a chair at the Charité until his death in 1847, formulated this as follows: „These in many cases doubtful, rarely only by the urge of circumstances varicose vein surgery is performed according to the various methods that have been recommended to be easier than to protect the patient from the adverse consequences of the same“.
The Lyons surgeon Charles Gabriel Pravaz injected in 1851 iron chloride solution in arteries and encouraged his students at the same time to try this method in varicose veins (3).
Theodor Billroth (2,3) also pointed out in his book in 1863 „General Surgical Pathology and Therapy.“ :
„We have to explain ourselves incompetently in the treatment of varicose veins, because we do not know of any means that would be able to destroy the disposition to these venous diseases… If we also removed one or more of these diseased veins, other paths would soon develop. For this only reason, I reject operations that have the purpose of removing one or more varicose nodules from the lower leg. Remember that the individual varicose veins themselves make almost no complaint at all, that any operation on the veins can become life-threatening through complication with thrombosis and embolism. So, I must consider the varicose vein operation to be completely unmotivated. Nevertheless, these operations are carried out especially in France and often with fatal outcomes.“
It is certainly justified to date the modern pathophysiology of venous insufficiency to Friedrich Trendelenburg (1844-1924). He introduced the concept of the „private cycle“ and thus founded the solitary ligature of the saphena to eliminate reflux. In 1891 he described his procedure in Brun’s contributions to clinical surgery under the title: „On the prevention of the saphenous vein magna in lower leg varicosities“ (36). At that time Trendelenburg was in Bonn, but had also worked at the University of Rostock from 1875- 1882.
Neither an extirpation of truncal varicose veins nor a crossectomy was associated with this procedure.

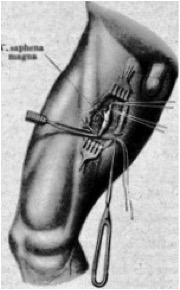
Friedrich Trendelenburg and his Varicose vein operation
He also processed the findings of Aquapendente from the 16th. century and those 100 years earlier from Rima to the ligature of the saphenous vein.
However, no extirpation of the trunk vein or crossectomy was associated with this procedure. The considerable number of recurrences prompted his former chief physician in Bonn, Georg Perthes, four years later to demand that the saphenous ligature be placed as far as possible proximally and that a saphenous segment should be resected (30).
Rostock can boast of another vein pioneer. In 1884, the Ordinarius Madelung (21) presented his method at the 13th Congress of the German Society of Surgery, in which the varicose vein side branches and perforators were extirpated from two skin incisions on the upper and lower leg as well as after back- preparation of both skin flaps in addition to truncal varicose veins. This method was practiced well into the 20th. century.
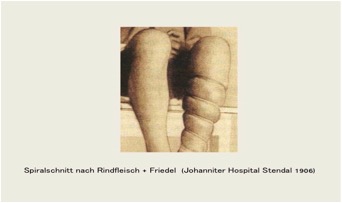
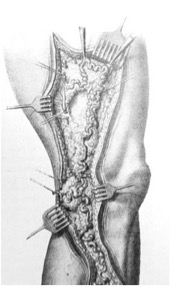
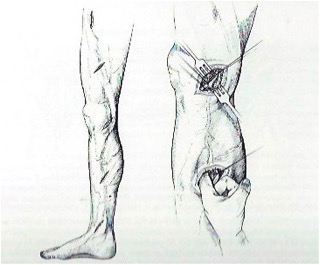
Op n. Rindfleisch, Op n. Madelung, Op n. Narath
Also worth mentioning are the spiral incision of the Stendal surgeon Rindfleisch 1906 (23,24) and the resection of the Utrecht surgeon Narath 1908 (28), often called „finger stripping“. He mobilized and removed the truncal varicose vein subcutaneously via several small skin incisions.
Numerous surgeons then attempted to eliminate saphena and its branches at the end of the 19th. and beginning of the 20th century. Most well – known were external compressions according to Schede, Kuzmik or Kocher, spiraling cuts, open deletion after Madelung and Narath resection (3).
Noteworthy, because much practiced at that time, is the percutaneous incisions and ligatures of varicose veins of the Swiss surgeon Emil Theodor Kocher. Per session up to 200 (!) incisions of veins were created on one leg (16, 42).
The instrumental removal of the truncal vein began with a kind of invagination of short vein segments by the American Keller in 1905 (13, 42).
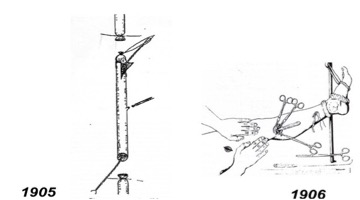
In 1906, Charles Mayo succeeded in the first promising saphenous extirpation in Rochester with a ring – curette developed by him, with which he triggered the extraluminal truncal vein (22, 42).
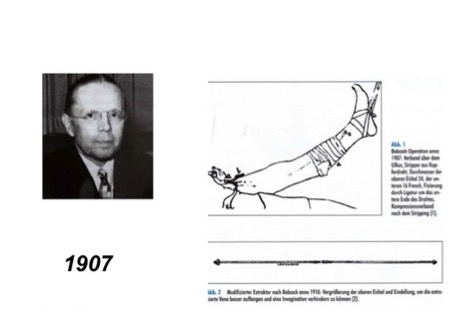
In 1907, William Wayne Babcock (1) was able to introduce the intravascular procedure with his stripper probe, which is still practiced today. However, the Mayo method, described in 1916 in Boston by John Homans with a combination of crossectomy, stripping and ulcer excision as radical surgery, remained the preferred method for many years (12, 42).
The first crossectomies that meet the demands of our day are attributed to the Italians Navaro and Moro (26) of Genoa around 1910 and the Boston John Homans (12) mentioned in 1916. The French surgeon Pierre Delbet of Paris suggested in his book „Surgery arterial et veineuse“ published in 1906, the transplantation of the saphenous vein in the femoral vein below the junction at the level of the first functional venous valve. He can be considered the founder of the valve plastic. However, this procedure has not been done frequently (3).
Saphenion®: The Endovenous „Saphena“ – The radically – the complications
The radical use of Saphena and the associated complications, admittedly, led to a limited spread of the stripping method in Germany in the first half of the 20th century.
There were numerous opponents who were even carried away by exaggerated statements. Let us quote the royal fountain doctor Professor Winkler from 1917 (11, 42):
„Babcock has indicated a method for cases where the dilated vein is rather straight, which surpasses everything that has been tried in this field in terms of crudeness. Before a patient gets involved in this graft, he should make his will“. Dermatologists, in particular, have tried to achieve varicose veins or chronic venous insufficiency by intravascular occlusion of the saphenous septum and its lateral branches.
Saphenion®: The Endovenous „Saphena“ – Begin of Sclerotherapy

The actual starting point of the sclerotherapy were observations during a lues epidemic in the First World War. Both the French dermatologist Jean Sicard, as well as the German Paul Linser (19,37) made the discovery that arm veins at the injection of Salvarsan deserted. This then led to the actual sclerotherapy on truncal veins and side branches. First, both doctors injected sublimate, then hypertonic saline. The successes of Linser and Sicard, as well as Sicard’s assistent Raymond Tournay brought the surgical procedures in the background. Also numerous surgeons left now the operational treatment. The method of Moszkovicz combined at least with an operative elimination of the Saphena as well as successes of the sclerosings made with the most different medications led M. Ratschow 1931 to the following statement: „The popularization of injection therapy, the sport and the fashion of the silk stocking have caused doctors to be swamped by younger patients as well. The varicose, almost always symptom – free in the initial stage and therefore not considered, were now perceived as a cosmetic defect „(31, 42).
Unfortunately, reports about recanalizations and critical opinions about the lack of long – term results of dermatologists became more frequent:
„Dermatologists always report on successes but rarely on long – term successes“, Moszkowicz complained in 1934.
And Zeller suggested already in 1927, „to combine „the well – founded bloody surgical therapy with the conservative method that is now so much in the process of being adopted“ (39, 42).
However, many years were to pass before the surgical therapy of the insufficient saphena was again accepted by the surgeons themselves.
Saphenion®: The Endovenous „Saphena“ – The Golden Twenties of Endovenous Saphena started.
Ferdinand Sauerbruch, director of surgery hospital Charitè Berlin since 1928, has banned his surgeons at Charitè hospital in 1929 all radical methods of varicose vein therapy (42)! There the surgeons used sugar sollution for sklerotherapy and sealing veins….He was followed by a lot of other collegues and directors in German hospitals…(42)
In 1932, a survey showed that 11 out of 12 surgical university hospitals in Germany performed sclerotherapy! Just after the Second World War did an increasing differentiation begin between cases suitable for sclerotherapy and classical truncal varicosis (42)
And so the Golden Twenties were the fist period of endovenous therapy of truncal varicosis veins and side branch varicose veins.

Saphenion®: The Endovenous „Saphena“ – After WW 2 – Differentiated therapy
The American babcock stripping process became increasingly popular after the World War 2. Contributing to this were:
– the development of flexible probes,
– the conscientious crossectomy,
– one required in particular by Hach – operation to protect healthy saphenous segments (8,9,10)
– the departure of coarse release varicose side branches towards mini incisions with the appropriate instrumentation as well
– the much improved diagnostics.
Unforgotten is the statement of the Nestor of German Vascular Surgery, Prof. Vollmar, at the Surgeons‘ Congress in 1969 that „the claim to sole representation of the sclerotherapy experts and leg wrappers as well as that of the exclusive strippers“. Nonetheless, it was an expression of the still subliminal rivalry between surgeon and dermatologist for professional competence with regard to the clinical picture. Unfortunately, the long standing disregard of many surgeons for the value of varicose vein disease has not helped us (38, 42).
Saphenion®: The Endovenous „Saphena“- Modernity in treatment of varicose veins
Later, surgeons and phlebologists developed the various endovenous techniques at the beginning of the 1990s again. Hence, they followed the demand of a nestor of phlebology, Urs Brunner, who already three decades ago formulated the desired treatment of Saphena as follows: „Today’s concept is conservative, reflux – oriented, aesthetic“.
It is easy to answer the question of what led to the rapid development of endovenous forms of therapy that today replace the stripping method:
– they avoid larger wound areas, haematomas and infections
– there is a general trend towards minimally invasive surgery
– the patients demand a rapid rehabilitation, preferably without inability to work as well as optimal cosmetic results.
– suitable technologies have been developed and modern catheter techniques also developed for phlebology
– also a preferably radical approach in the conventional varicose vein surgery could not prevent the recurrence, with the actual recurrence rate after operative remediation of truncal varicose veins has not yet been clearly proven. The information on this varies between 7 and 60 per cent (5, 6, 7, 42).
Saphenion®: The Endovenous „Saphena“ – The conclusions
And so, through the use of the new procedures adapted to the findings, the Saphena’s long path of suffering also seems to have come to an end, in which it can remain closed but without damage to the surrounding structures and for the benefit of its bearers in its traditional place. The Golden Twenties were playing an very important role in development of endovenous therapy and in think about non radical therapeutic ways of therapy
We would like to conclude with Rudolf Klapp’s statements made in 1923 and still valid today, at that time Head of the Surgical university ambulance in Berlin:

„In the case of a pains so widespread as the varicose veins are, the operative treatment would have to be so successful that a patient who is satisfied with the operation always sends 10 others. “ Rudolf Klapp, 1923 (14,15,42).
Photos / Videos: Utzius
References:
1. Babcock WW, New York Medical J 1907;86:153-156
2. Billroth Th, Die allgemeine chirurgische Pathologie und Therapie, Berlin: Reimer 1880
3. Budde, Werner; Rehn, Eduard; Rothe Gerhard:Operationen an den Blutgefäßen in Bier, Braun, Kümmell: Chirurgische Operationslehre, J. A. Barth, siebte Auflage 1958, Band 6, 353 – 358
4. Dieffenbach J.F. , Die Operative Chirurgie , Erster Band, Leipzig, F.A. Brockhaus , 1845
5. Dwerryhouse S et al J Vasc Surg 1999;29:589-92
6. Fischer R et al, Phlebologie 2000;29:17-22
7. Fischer R et al, J Vasc Surg 2001;34:236-40
8. Hach W, V. Hach-Wunderle, Die Rezirkulationskreise der primären Varikose; Springer Berlin,Heidelberg,New York, 1994
9. Hach W , Gefäßchirurgie 2001;7:111-118
10. Hach W, V.Hach-Wunderle, Phlebologie 2008;37:55-60
11. Hohlbaum G G, Phlebologie 1998;27:138-46 und 171-179
12. Homans J. The operative Treatment of varicose veins and ulcers. Surg Gyn“c Obstet 1916; 22: 143 – 58.
13. Keller W, New York Medical J 1905;82:365
14. Klapp R. Über Krampfaderbehandlung. Klin Wschr 1924; 3:156 – 8.
15. Klapp R. Fortschritte in der Behandlung der Krampfadern. Fortschr. Therap 1930: 39 – 42
16. Kocher T. Vereinfachung der operativen Behandlung der Varicen. Dtsch Zschr Chir 1916; 138: 113 – 151.
17. Lahl W et al, Dt Gesundh Wesen 1979;34:2184-89
18. Lehmann G M, Die verwendung der Lövqvistschen Rollmanschette bei der minimalinvasiven Varizenchirurgie; Inauguraldiss Uni Bonn, 2003
19. Linser-Vohwinkel-Schneider. Moderne Therapie der Varicen,Hämorrhoiden und Varicocele 3.Aflg. Stuttgart: Enke 1955.
20. Lövqvist J, Chirurg 1988;59:853-854
21. Madelung O, Verh Dtsch Ges Chir 1884;13:114-117
22. Mayo CH. Treatment of varicose veins. Surg Gynaec Obstetr
1906: 385 – 8.
23. Meyer F. Die Behandlung des varikösen Symptomenkomplexes nach Rindfleisch-Friedel und deren Erfolge. Btrg klin Chir. 1914; 89: 276 – 89.
24. Meyer FG. Zur Varizenbehandlung, insbesondere nach Rindfleisch. DMW 1924: 1410 – 1.
25. Minkiewicz J. Vergleichende Studien über alle gegen Varicen empfohlenen Operationsverfahren. Arch pathol Anat u Physiologie u klin Med 1862; 25: 193 – 267 u. 1869; 45: 409 – 44.
26. Moro G, Beitr klein Chir 1910;71:420
27. Moszkowicz L, Zentralbl Chir 1927;54:1732-1736
28. Narath A, Dtsch Z Chir 1906;83:104-110
29. Negus D, Br J Surg 1993;80:823-4
30. Perthes G. Ueber die Operation der Unterschenkelvaricen nachTrendelenburg. DMW 1895: 253 – 7.
31. Ratschow M. Über die kausale Genese der Varicenkrankheit. Klin. Wschr 1931; 10: 2226 – 8.
32. Sam R C et al, Eur J Vasc Endovasc Surg 2004;27:113-120
33. Schadeck M, Phlebologie, 2017;46:55-59
34. Schede M, Klein Wochenschr 1877;14:85-89
35. Stemmer, Robert: Die Varizenverödung; Ganzonie & Cie AG 1988
36. Trendelenburg F, Beitr Klein Chir 1891;7:195-210
37. Van der Molen H R , Phlebologie 1981;34:313-32.
38. Vollmar J, Langenbecks Arch Chir. 1969;325:669-672
39. Zeller A, Zur Behandlung der Varizen. Jahresks Ärztl Fortb1927; 18: 1 – 9
40. Zierau, Ulf Thosten; https://www.saphenion.de/news/arbeiten: rostocker-chirurgen – in-der-geschichte-der-gefaesschirurgie/
41. Zierau, Ulf Thorsten: Die Geschichte der Gefäßchirurgie in Berlin, vasa 1995
42. Lahl, W und U Zierau: The fate of „Saphena“ – Views into the Past; JVET, 2018; Vol.3, No.4:23
Scientific References
S 1: Almeida et al.: Recovery Trial – Final Results;J. Vasc. Interv. Radiol.; June 2009.
S 2: Almeida J. I.: Current State of Endovenous Ablation; Endovascular Today, October; 2007; 73 – 76.
S 3: Almeida J.I.: Options for Treating the Saphenous Vein; Endovascular Today, March; 2006; 36 – 39
S 4: Boros, M.J. et al.: High ligation of the saphenofemoral junction in endovenous obliteration of varicose veins. Vas. Endovascular Surgery 2008; 42; 235 – 238.
S 5: Fleck, Klaus: Bye bye Stripping: Zur Behandlung von Varizen ist der Katheter oft die bessere Wahl; med scape, 7.12.2018
S 6: Gibson, K. et al.: Need for adjunctive procedures following cyanoacrylate closure of incompetent great, small, and accessory saphenous veins without the use of postprocedure compression: Three-month data from a postmarket evaluation of the VenaSeal System (the WAVES Study). Phlebology, 2018,
S 7: Goode S. et al.: A Randomised study comparing Endovenous Laser Ablation and Radiofrequency Ablation for the treatment of varicose veins; 22nd. NICE – meeting, ESVS, 2008.
S 8: Hamann, SAS. et al.: Editor’s Choice – Five Year Results of Great Saphenous Vein Treatment: A Meta-analysis. Eur. J. Vasc. and Endovasc. Surg. 54 (2017), 760 – 770
S 9: Lahl, Wolfgang und Zierau, Ulf Th.: Laserbehandlung bei Varicosis -Technik und Ergebnisse; chirurgische praxis, 69 (2008); 267 – 278
S 10: Lawaetz, M. et al.: Comparison of endovenous ablation techniques, foam sclerotherapy and surgical stripping for great saphenous varicose veins. Extended 5-year follow-up of an RCT. Int. Angiol. 2017; 36; 281 – 288.
S 11: Mackay, E.G. et al.: Saphenous Vein Ablation – do different wavelength translate into different patient experiences; Endovascular Today, March 2006; 45 – 48.
S 12: http://www.phlebology.org/member-resources/clinical-guidelines
S 13: Paravastu SC. et al.: Endovenous ablation therapy (laser or radiofrequency) or foam sclerotherapy versus conventional surgical repair for short saphenous varicose veins.
S 14: Park. I.: Initial Outcomes of Cyanoacrylate Closure, VenaSeal System, for the Treatment of the Incompetent Great and Small Saphenous Veins. Vasc. Endovascular Surgery, 51 (2017); 545 – 549
S 15: Proebstle, Th. et al.: Endovenous ablation of refluxing saphenous and perforating veins. VASA 2017, 46; 159 – 166
S 16: Tekin, A.L. et al.: Nonthermal, Nontumescent Endovenous Treatment of Varicose Veins. Ann. Vasc. Surg.36 (2016), 231 – 236
S 17: Wittens, C. et al.: Editor’s Choice e Management of Chronic Venous Disease Clinical Practice Guidelines of the European Society for Vascular Surgery (ESVS); Eur. J. Vasc. Endovasc. Surg. (2015) 49; 678 -737
S 18: https://www.nice.org.uk/guidance/cg168
S 19: http://www.phlebology.de/leitlinien-der-dgp-mainmenu/280-leitlinie-zur-diagnostik-und-therapie-der-krampfadererkrankung#kap10_3
S 20: Timperman, Paul E.: Prospective Evaluation of Higher Energy Great Saphenous Vein Endovenous Laser Treatment; J. Vasc. Interv. Radiol.2005; 16; 791 – 794
Both autors, Dr. Zierau and Dr. Lahl, have no conflict of interest!
Dr. U.Th.Zierau, Dr. W.Lahl
Saphenion® Vascular Center Rostock,