Saphenion®: Muscle vein varicosis and intermittent claudication – real risk for arteries?
Saphenion®: Muscle vein varicosis and intermittent claudication – is there a risk of arterial blood flow? This is very interesting and also for our patients and the vascular and vein specialists a very important question. Because varicose muscle veins are signs of advanced varicose vein disease of the skin veins and the perforator / connecting veins. Important too – muscle veins do not carry venous valves, so they can not defend themselves against the pathologically high pressure of the varicose veins.
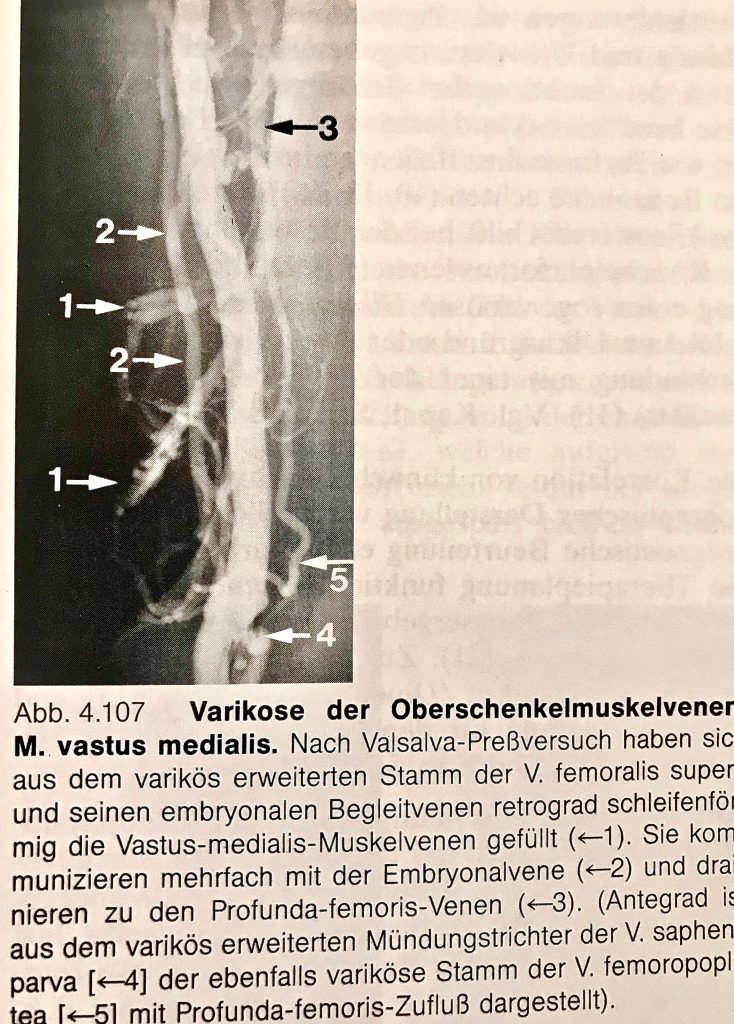
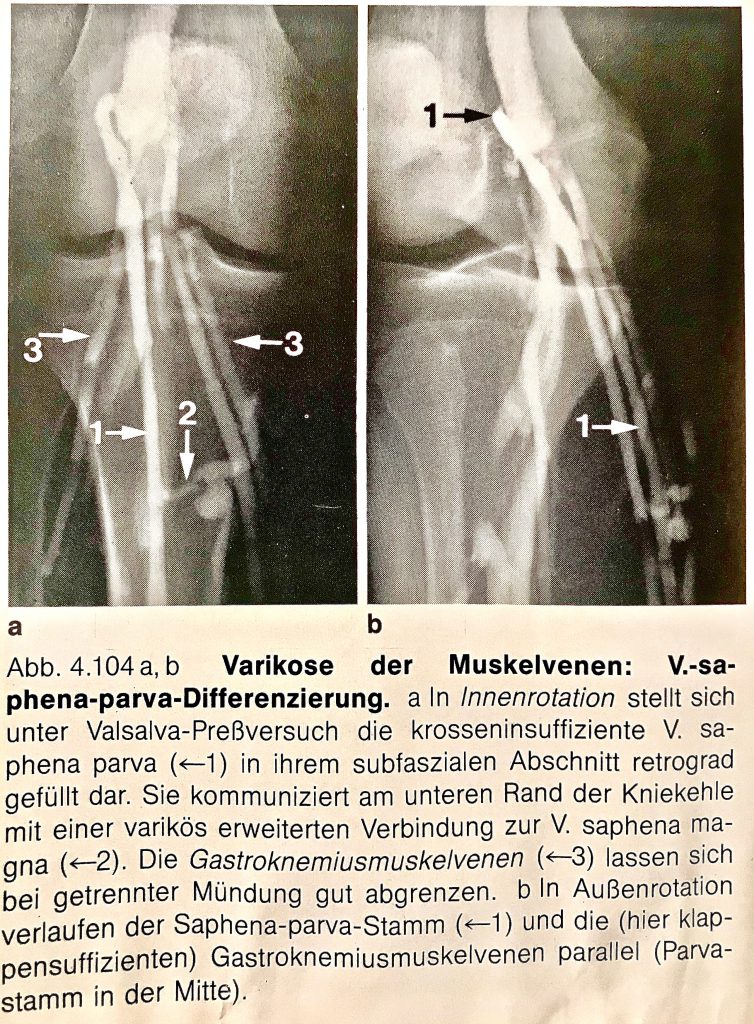
Saphenion®: Muscle vein varicosis and intermittent claudication – Old phlebographic images showing the varicosis – also varicose muscle vein varicosis were visible.
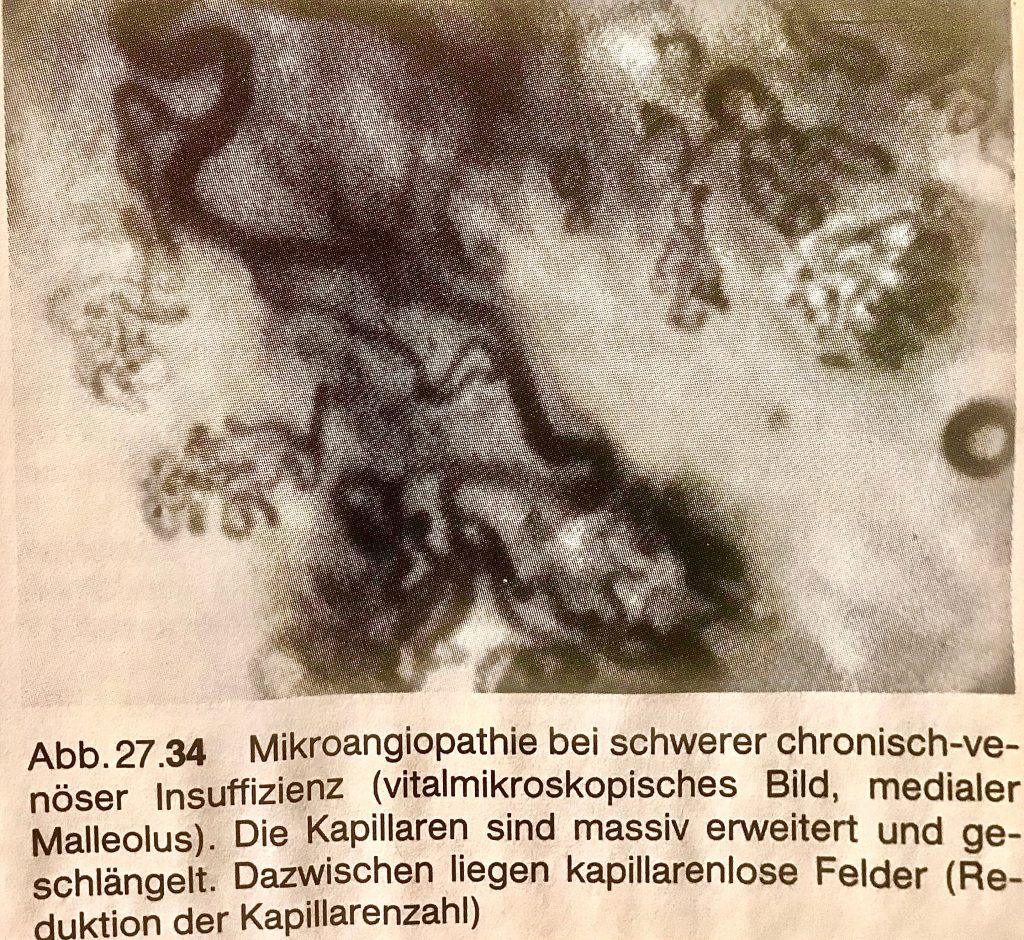
This advanced varicose vein disease results in heavily dilated muscle veins via a truncal varicose vein and connecting varicose veins. This then constant venous hypertension in all upright positions (even when sitting!). Affects extremely unfavorable to the end stream of the arterial and venous vessels – the arterioles, capillaries, and venules -. At an advanced stage, it is possible to detect markedly strong microangiopathy of the capillaries. These are greatly expanded and meandered.
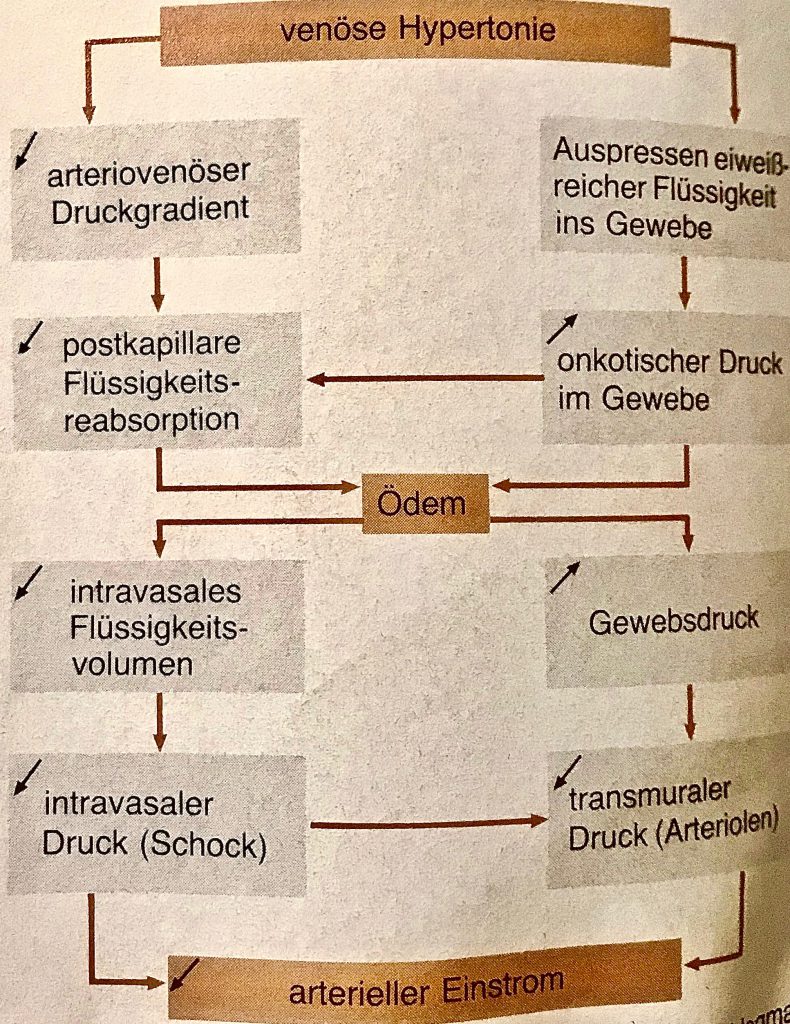
From the damaged capillaries, which are supposed to bring the oxygen-rich blood into the muscle via perfusion, large quantities of protein-rich fluid escape into the interstitium. The capillary wall is often permeable to pressure so that complete cellular elements are perfusing (e.g., red blood cells). These are degraded to visible brown hemosiderin deposits in the tissue.
Saphenion®: Muscle vein varicosis and intermittent claudication – oxygen pressure as low as the heavy smoker’s leg
In clinical studies of severe venous insufficiency, oxygen pressures were measured that were as deep as in a heavy smoker’s leg (syn: intermittent claudication).
In extreme cases, it can lead to severe skin changes up to the open leg (ulcera crures). Also, load-dependent pain of the calf muscles, limited performance during physical exercise, and a fast and tiring long time muscle can be felt (competitive sports!).
Thus, it is an urgent need, in the search for varicose veins by duplex sonography also represent the muscle veins and to weight accordingly functional. As venous specialists, we must also inform the patient of this, as there are no purely cosmetic symptoms or signs of swelling in the summer months.
Saphenion®: Muscle vein varicosis and intermittent claudication – clinical examination and therapy
The first item is the question of anamnesis and pain. The clinical examination usually leads to the detection of a defective perforator/ communicating veins. Now, however, it is also important to examine, present, and evaluate the most endangered venous valveless muscle veins. This is very well possible today with duplex ultrasound, whereas it was not always possible to represent it reliably in venography (venous radiography with contrast medium).
If there are dilated and varicose muscle veins, we must assume a peripheral capillary – also arterial – circulatory disorder and communicate this to the patient.
There is a significantly increased risk of the already mentioned complications – including a load restriction of the lower leg muscles. However, this is also a significant component in professional active and competitive sports.
A fairly rapid rehabilitation of the truncal varicose veins, lateral veins but also connecting veins is quite urgent. To what extent the varicose muscle veins are also accessible to direct therapy should be feasible with the now-established minimal-invasive varicose vein therapy using sealing foam or vein glue (venaSeal®local therapy).
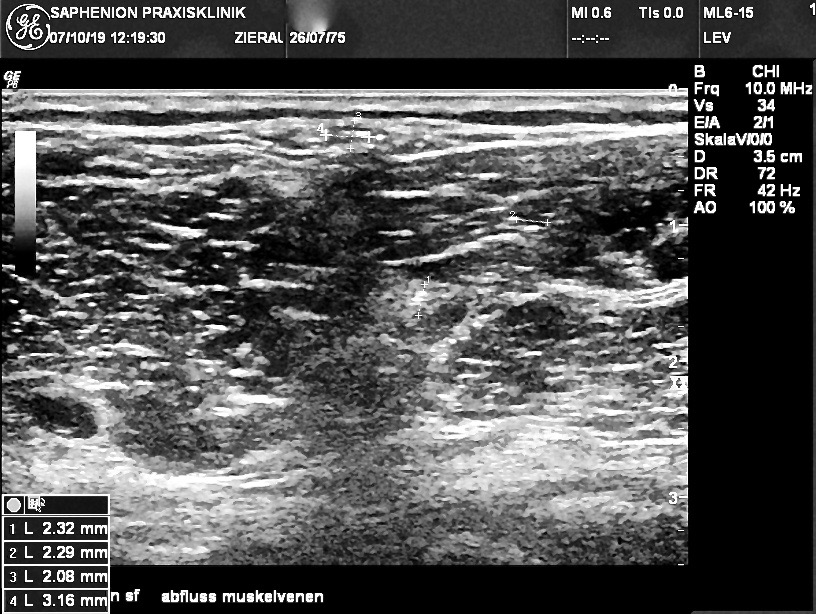
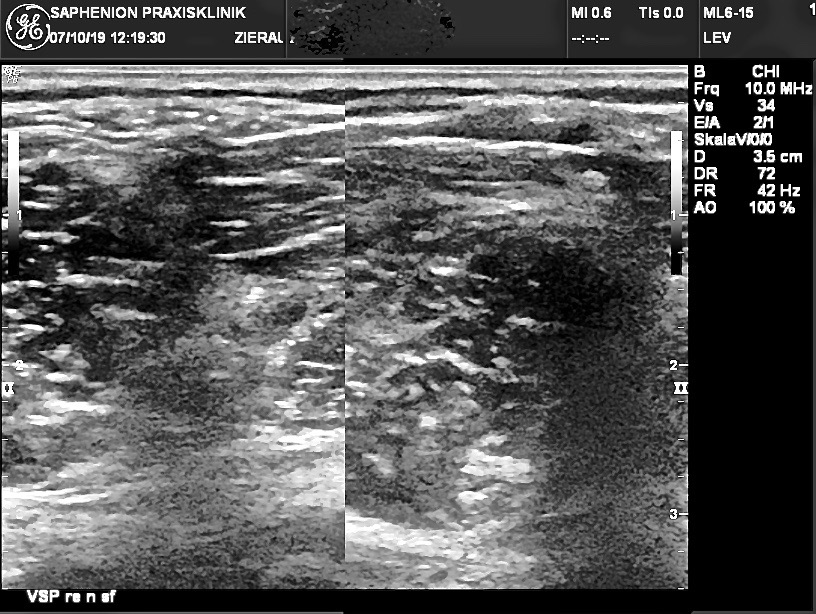
Saphenion®: Muscle vein varicosis and intermittent claudication – Ultrasound lower leg with dilated muscle veins (right picture). After Sealing the Foam, foam is floating also inside the dilated muscle veins (left picture)
Saphenion®: Muscle vein varicosis and intermittent claudication – Thrombosis prophylaxis in microfoam therapy?
Is thrombosis prophylaxis in the case of microfoam therapy indicated on the lower leg? In our more than 20400 duplex ultrasound-guided microfoam treatments, we were also able to show a filling or outflow of microfoam via the muscle veins on the lower leg in some cases.
Therefore, SAPHENION® uses foam on the lower leg and side branch/truncal/perforant varicosis to prevent the risk of muscle vein thrombosis under Intra therapeutic thrombosis prophylaxis.
Saphenion®: Muscular vein varicose veins and intermittent claudication – Oxygen – multistep – therapy after the catheter therapy of varicose veins
According to the initial question of our article, we also thought about whether oxygen-multi-step – therapy accompanying the treatment of varicose veins is useful. On the one hand, to increase the oxygen concentration in the muscle, on the other hand, to raise and balance the reduced arterial concentration, especially in the arteries of the lower leg, due to the increased venous pressure.
We decided 42 months ago to offer this concomitant therapy to our patients. We perform this therapy in parallel with postoperative compression massage. We have been performing vacuum massage therapy for 9 years after every minimally invasive catheter procedure, whether VenaSeal®, radiofrequency catheter, or microfoam.
The massage therapy lasts 20 – 30 minutes, the oxygen therapy is used during the whole course of the massage. At the beginning of the oxygen therapy and at the end of the therapy cycle, we measure the initial value of the oxygen partial pressure and the achieved therapeutic value on hand and foot, as already described, and document them in our therapy protocol. The oxygen masks remain with the patient for further sessions (sustainability requirement!) – we do not clean them or use them again on another patient.
The aim is, besides the normalization of the venous pressure and the reduction of the tissue pressure, also to achieve an improvement of the blood-oxygen content, in order to improve the microcirculation in the legs in a sustainable and multifactorial way.
In our 40-month results, a reduction of immunological tissue reactions as well as a thrombosis-induced cell reaction to both the vein glue VenaSeal® (4.1% to 6.9% of all treated cases) and the microfoam (0.8% to 1.9% of all treated cases) was observed in every case.
Together with a coupled decongestion therapy through vacuum compression, faster healing with comparatively significantly lower side effects and discomfort can be achieved and proven with the use of SMT post-therapeutically.


Photos: Utzius
Pathologisches Museum Charitè
Siegenthaler: Pathophysiologie
Weber, May: Funktionelle Phlebologie
Literature / Links:
Siegenthaler, W.: Klinische Pathophysiologie; Georg Thieme Verlag Stuttgart New York 1987.
Weber, J. und May R.: Funktionelle Phlebologie; Georg THieme Verlag Stuttgart, New York, 1990.
Danneil,O.; C.Kern und M.Stücker: Tiefe Muskelvenenthrombose nach Sklerosierung eines Seitenastes unter laufender Therapie mit Tamoxifen; vasomed 5, 2019.
http://www.ejves.com/article/S1078-5884(15)00097-0/abstract
http://www.ncbi.nlm.nih.gov/pubmed/26557230
http://www.ncbi.nlm.nih.gov/pubmed/23864535
http://gesundheitsnews.imedo.de/news/1017861-krampfadern-minimalinvasive-therapien-auf-dem-vormarsch
http://www.ncbi.nlm.nih.gov/pubmed/26384639
http://www.ncbi.nlm.nih.gov/pubmed/26036246
